BY: SREELAKSHMI (MSIWM012)
An emerging field of medicine called regenerative medicine or cell therapy refers to treatment derived from the idea of producing new cells that will replace malfunctioning or damaged cells as a vehicle for the treatment of diseases and injuries. The focus is on developing effective mechanisms for stem cell replacement. This is especially beneficial for age-related diseases such as Alzheimer’s disease, Parkinson’s disease, type II diabetes, heart failure, arthritis, and aging of the immune system. It is believed that replacing damaged or dysfunctional cells with full functionality could be a useful treatment strategy in the treatment of many of these diseases and conditions.
Different Types of Renewable Medicine
Cell Therapy
Each of the 200 integrated cells in the human body is derived from one cell which is the fertilized egg. As the fertilized egg grows, it forms embryonic stem cells, each of which has the potential to form the different types of cells found in adults and are organized into structures that will become tissues and organs. But some live in an inseparable state with older stem stem cells that can be transformed into a limited range of cell types.
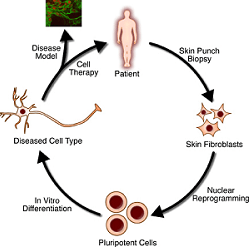
Remedies that use patients’ cells to regenerate their organs or tissues are called spontaneous therapies. Methods include ongoing testing at two London hospitals to treat 100 heart attack patients with stem cells in their bone marrow to help repair damaged heart tissue. Therapies that use cells or tissue derived from a non-patient patient are called allogeneic therapies. Examples include the use of bone marrow or stem cells from similar donors or the use of ES cell lines established for treatment.
Tissue Engineering
The term “engineering tissue” came into use in 1985, by Y. Fung, a pioneer in the field of biomechanics and bioengineering, also stated that Tertiary engineering is a multidisciplinary field that uses the principles of engineering and health science to improve biological processes that restore, maintain or improve tissue function.” Tissue engineering modifies the cells or tissues in some way in order to repair, regenerate, or regenerate tissue. Perhaps the most well-known example of this was the process of trachea formation for a patient with airways that had been severely damaged by tuberculosis. Other examples of tissue engineering include artificial skin, which is made using human cells (fibroblasts) implanted in a matrix of proteins (fibrin) and cartilage membranes to be implanted in patients who have ruptured the cartilage of the knee.
Tissue engineering at its basic level fills the scaffolding of 3D tissues (biomaterials) by cells to produce functional organ formation. Tissue engineering aims to address the latest shortage of critical organs through the formation of living organs.
Biomedical Engineering
Another form of self-rehabilitation therapy is to make biomedical devices that mimic the function of tissue or organ. For example, Type 2 diabetes results in the destruction of beta-producing insulin-producing cells. Patients with this type of diabetes should monitor their blood glucose levels regularly and inject the hormone insulin to keep the level normal. While some research teams are working to restore beta cell functionality they are using biomedical engineering to improve artificial limbs. Using ultra-low power electronics originally designed for mobile phones, they developed a small built-in glucose sensor chip that can be inserted into a patient. The chip would regularly monitor blood glucose levels, produce the high amount of insulin needed to maintain stable glucose levels and send wireless signals to the pump to release the right amount of insulin.
Genetic Therapy
Although there are a variety of genetic therapies, the most obvious is to identify a medical condition that can be treated with a specific protein, and then introduce genetic code into that protein in the affected cells. In practice, finding genes that work in cells with the result of continuous treatment is extremely difficult. Nevertheless, in recent years there has been some progress in the use of genetic therapy to regenerate tissues, especially in the area of heart disease.
Stem cells and Regenerative medicines
Stem cells have are able to develop into many types of cells in the body. They can act as a kind of immune system they can also differentiate without limit to fill other cells. When a stem cell divide, the new cell obtained has the ability to reside as a stem cell or into another type of cell which are having specific functions it can turn out to be like a muscle cell, a red blood cell, or a brain cell. There two types of stem cells: embryonic stem cells and adult stem cells. Embryonic stem cells are found in embryos and the sources of adult cells are the umbilical cord, menstrual blood, muscles, tendons, adipose tissue, bone marrow etc. a group of adult stem cells can be incorporated in vitro or in vivo to separate osteoblasts, chondrocytes, adipocytes, tenocytes, myotubes, neural cells and stroma supporting hematopoietic. The sheer strength of these cells, their easy separation from culture, and their extremely high ex vivo power make these cells an attractive therapeutic tool in reconstructive medicine.

Recent Advancements in Regenerative Medicine
- Direction of cell expansion and differentiation, which explains the processes of how tissues and organ grow.
- Development of techniques for assembly of cells into large, three dimensional tissue-like structures, which will lead to the physical creation of three dimensional organs.
- Custom-designed biomaterials to serve as structural templates for tissue development, which helps scientists build organs.
- Automated bioreactor culture vessels, which allow scientists to mass produce cells and tissues.
