BY: Ria Fazulbhoy (MSIWM031)
How does it occur?
This disease is currently the leading cause of death, worldwide. The ischemic heart disease is also known as coronary artery disease (CAD), atherosclerotic heart disease and coronary heart disease (CHD).
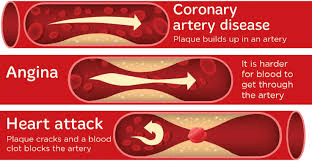
The disease occurs due to the blockage of the arteries leading to inadequate blood supply to the heart due to a number of reasons like building of plaque, excess exertion, high levels of cholesterol, etc. While narrowing may be caused by a blood clot or blood vessel constriction as well, it is more often caused by plaque accumulation, called atherosclerosis.
In the blood, cholesterol particles begin to accumulate on the walls of the arteries that supply the heart with blood. Eventually, it can form deposits called plaques. These deposits narrow the arteries and obstruct the flow of blood eventually.
The amount of oxygen supplied to the heart muscle is decreased by this reduction in blood flow. The heart muscle cells die, which is called a heart attack or myocardial infarction, when the blood supply to the heart muscle is completely blocked (MI).

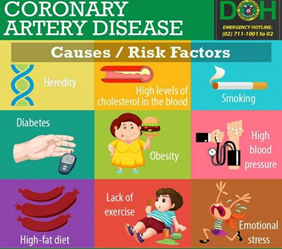
Risk factors that increase chances of the disease:
The risk of developing ischemic heart disease is raised by a variety of variables. Not all individuals with risk factors are going to get ischemic heart disease. There are risk factors for ischemic heart disease include:
- Diabetes
- Family history of the condition of the heart
- High cholesterol in the blood
- Blood Pressure High
- Strong triglycerides in the blood
- Obesity
- Inactive physique
- Smoking and other forms of tobacco
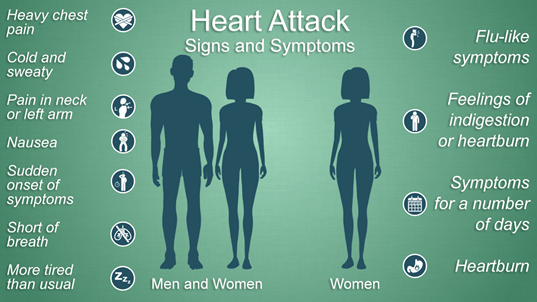
Symptoms:
People can experience ischemic heart disease symptoms either regularly or only occasionally, depending on the severity of the case. Some common symptoms experienced by patients include:
- Angina pectoris
When the heart muscle is deprived of enough oxygen, the pain endured is called angina pectoris. This is a clinical condition characterized by chest, chin, shoulder, back, or arm pain that is normally exacerbated by exercise or emotional stress and immediately relieved by rest or nitroglycerin use.
- Breath shortage: One can experience shortness of breath or severe exhaustion with exercise if the heart can’t pump enough blood to meet the needs of your body.
- Heart attack. A coronary artery that is totally blocked can cause a heart attack. Crushing pressure in one’s chest and pain in your shoulder or arm, sometimes with shortness of breath and sweating, are the classic signs and symptoms of a heart attack.
- Arrhythmia – abnormal heart rhythm: Inadequate blood flow to the heart or heart tissue damage can interfere with the electrical impulses of your heart, causing irregular heart rhythms.
Diagnosis:
- Electrocardiogram – ECG or EKG: The electrical activity, rate, and regularity of your heartbeat are calculated by
- Echocardiogram: A image of the heart is generated using ultrasound (special sound wave).
- Exercise stress test: Tracks your heart rate as you walk on a treadmill. This helps to decide how well the heart functions as more blood needs to be pumped.
- Chest X-ray: In order to create an image of the heart, lungs, and other organs in the chest, x-rays are used.
- Coronary angiogram: Monitors blockage and passage of blood into the coronary arteries. In order to detect dye injected through cardiac catheterization, X-rays are used.
- Coronary artery calcium scan: A computed tomography (CT) scan searches for calcium accumulation and plaque in the coronary arteries.
Treatment:
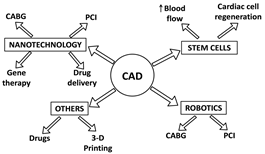
Treatment given to patients suffering from Ischemic heart disease can include drug therapy, regular exercise, quitting of smoking/ tobacco, healthy dietetic.
Medications used to treat the disease include:
- Angiotensin-converting enzyme (ACE) that relax blood vessels and decrease blood pressure.
- Angiotensin receptor blockers (ARBs) which help in lowering the blood pressure.
- Anti-ischemic agents like ranolazine, for example (Ranexa)
- Antiplatelet drugs that stop blood clots from forming
- Beta-blockers that decrease the heart rate
- Calcium channel blockers that lower the heart muscle workload

